Understanding the direct impact of nutritional and lifestyle changes on presenting symptoms, particularly regarding mental health, is challenging. There's a pressing need for improved strategies to prevent and support recovery from mental illness, which remains the leading cause of disability worldwide.
Practitioners today have access to a comprehensive toolkit to aid decision-making. This includes functional testing to identify imbalances and deficiencies, as well as diagnostic evidence to guide interventions. Strategies like the adoption of using food sensitivity testing to inform a personalised anti-inflammatory diet, tailored with functional foods such as green tea, blueberries, or cocoa allow for more precise dietary recommendations.
Perhaps the most crucial tool is the recording of symptoms by patients. Personal engagement in intervention strategies fosters interest and compliance, enabling daily tracking of effects on mood, energy, and sleep. This data provides a broader health perspective that clients can directly relate to. With numerous portable health tech devices and apps available, monitoring health and tracking activity has never been easier.
Emerging evidence suggests that our food choices significantly impact mental health risk. For instance, studies like the Smiles Trial indicate that nutritional interventions can lead to direct improvements in mental health, highlighting the potential of nutritional psychiatry.
Clinical case study
Presentation
David, a 66-year-old man, presented with severe joint pain and anxiety. Despite his life seeming stable, he felt low and was prescribed amitriptyline by his GP. To counteract his low mood, David took regular exercise daily.
Initial consultation
David began a generic anti-inflammatory diet (AID) rich in healthy fats, lean proteins, and plant-based foods. His vitamin D levels were tested, revealing a deficiency that can lead to fatigue, anxiety, and slower wound healing. He was advised to take 4,000 IU of vitamin D daily for two months and retest after three months.
His AID was further tailored using IgG testing to assess reactions to over 200 foods.
Test results
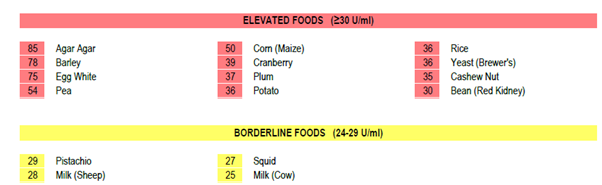
The five most reactive foods were eliminated for three months. Notably, high-sugar vegan ice cream was identified as the source of agar agar. Gradual reduction of sugar was implemented, transitioning from dates to phytonutrient-rich fruits to increase fibre consumption.
David maintained a diverse diet while other foods were rotated and consumed twice a week. He was encouraged to exercise at moderate levels, and seek psychotherapy for anxiety management. He returned to his GP for further assessments, which showed no additional issues.
Follow-up one
After two months, David reported significant improvement in joint pain and anxiety, better sleep, and reduced morning discomfort.
Follow-up two (one year later)
David’s symptoms flared as his sugar intake increased. He was advised to restart his original AID. Testing revealed elevated hs-CRP levels at 7mg/L indicating increased inflammation. Scores of 3.1 mg/L or over are considered high risk for cardiovascular and metabolic disease. An adrenal stress test highlighted high cortisol and low DHEA, indicating a catabolic state, likely exacerbating his symptoms.
See his first 3 cortisol samples testing his Cortisol Awakening Response (CAR) below. The CAR response measures waking cortisol and the immediate anticipated response to the stressors of the day ahead. Ideally, sample 3 should drop to within ‘normal’ ranges and decrease gradually throughout the day.
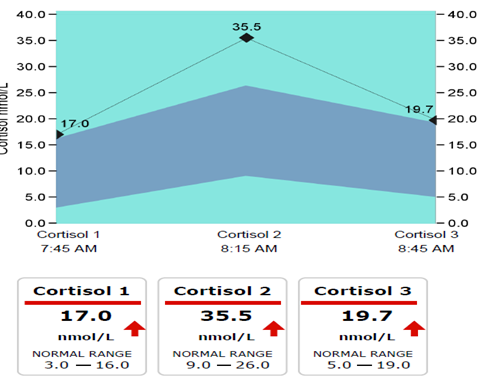
David was in an ‘alarm’ state, his high cortisol response being sustained throughout the day. His body was working hard to sustain the stress response thus diverting energy away from normal metabolic processes.
Follow-up three (three months later)
David felt revitalised after starting corticosteroid treatment for a diagnosis of reactive arthritis and implementing dietary and lifestyle strategies. He had stopped taking amitriptyline and was actively engaged in his psychotherapy sessions, expressing optimism and experiencing less pain.
Follow-up four (18 months after initial testing)
After IgG retesting, David’s ‘healthier’ diet revealed some unexpected results. Despite focusing on anti-inflammatory foods like flaxseed and fish, he found these may have been actively contributing to inflammation.
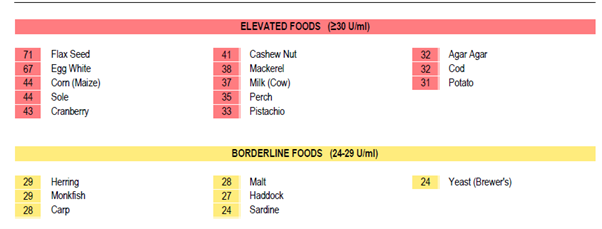
His elevated egg white score indicated incomplete avoidance of eggs. He identified a cross-reaction between cranberries and blueberries, which he had added to his porridge daily. Food alternatives were easily found.
David’s second hs-CRP test showed improvement, dropping from 7 to 2.5 mg/L, illustrating the effectiveness of combining dietary, lifestyle, and medication interventions in improving mental health and, specifically, joint pain.
Defining mental health
Mental health encompasses a person’s overall psychological well-being, including emotional, social, and cognitive functioning. It is essential for coping with life's stresses, productivity, and societal contribution. David’s case highlights how nutrition directly influences mental health symptoms.
Research has established links between inflammatory cytokines and mental health disorders. Testing for inflammation levels and regulating these responses can facilitate tissue repair and alleviate symptoms, supporting a return to homeostasis. An unregulated inflammatory response can negatively impact neurocognitive function by disrupting the blood-brain barrier.
The blood-brain barrier, a semi-permeable membrane, is less protective and more vulnerable to peripheral inflammation than was previously thought. It acts as a bidirectional communication system between the innate immune system of the brain and the peripheral immune system. Increased peripheral immune system activity chronically activates the specialised macrophages of the brain parenchyma known as microglia, promoting blood-brain barrier breakdown. This breakdown may allow peripheral inflammatory mediators to enter the central nervous system, increasing neuroinflammation and the risk of neurocognitive diseases.
Anti-inflammatory diets significantly reduce the risk of chronic diseases, and personalised approaches through testing can enhance their effectiveness.
To explore these concepts further, watch our recent webinar, The Mind-Body Connection: How Food Sensitivities Impact Cognitive Health.
Conditions linked to mental health
Several conditions associated with mental health include anxiety disorders, mood disorders, personality disorders, psychotic disorders, eating disorders, and substance abuse disorders. It’s common for individuals to experience symptoms from multiple mental illnesses simultaneously.
The link between mental health disorders and food immune responses
Research indicates that an IgG-guided diet based on food sensitivity testing may lead to a 78% improvement in symptoms.

Inflammation could be a key factor connecting physical and psychological symptoms, mediated by cytokines—chemical messengers of the immune system. Changes in behaviour associated with depression arise from the interaction between pro-inflammatory cytokines produced in both the peripheral and central nervous systems and the neuroendocrine system. This interaction can activate the hypothalamic-pituitary-adrenal (HPA) axis. Elevated levels of pro-inflammatory cytokines are linked to the development of neuropsychological and somatic symptoms of depression, with interleukin-1 and TNF-alpha found to be elevated in the cerebrospinal fluid of individuals with depression.
Moreover, there are established connections between inflammatory diseases—such as asthma, COPD, diabetes, allergies, and rheumatoid arthritis—and depression.
Diagnostics tests from CNSLab
Ready to get a food sensitivity test?
Browse our FoodPrint® home to lab test kits to find the most suitable option.
Gut barrier dysfunction and inflammation
Lifestyle-related gut barrier dysfunction may contribute to conditions like migraines by compromising the gut epithelial wall. This allows undigested proteins to trigger inflammatory responses. Research has shown that individuals with frequent migraines exhibit higher levels of food allergens increased IL-6 and TNF-alpha, and worse anxiety and gastrointestinal symptoms.
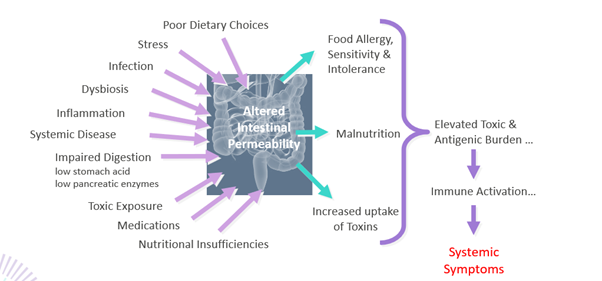
Stress also plays a disruptive role, as cortisol-releasing hormone (CRH) affects mast cell degranulation and the release of pro-inflammatory mediators, leading to neuronal effects. Mast cell activation can impair both the gut barrier and the blood-brain barrier, facilitating the entry of toxins and immune cells and exacerbating inflammation. Neuroinflammation is increasingly recognised as a key factor in diseases like multiple sclerosis and other neurodegenerative conditions.
Depression has been linked to neurotransmission changes in the central nervous system, resulting in structural brain changes due to neuroendocrine, inflammatory, and immunological mechanisms. IgG food hypersensitivity may significantly contribute to these issues.
The role of gluten and food sensitivities
Gluten can negatively influence inflammation and may be a critical factor in the development of mental health disorders. Gliadin, a component of gluten, can lead to excessive zonulin production, which loosens the tight junctions of the gut barrier, potentially causing leaky gut and promoting the release of pro-inflammatory cytokines. Even brief exposure to gluten can trigger symptoms resembling depression in sensitive individuals.
If food-specific IgG hyperreactivity is more prevalent among patients with irritable bowel syndrome (IBS) and major depressive disorder (MDD) than in healthy individuals, it makes sense to test for foods that provoke and sustain immune responses in clients with these conditions.
Research has also associated elevated IgG antibodies to foods with schizophrenia and autism spectrum disorder (ASD). particularly concerning wheat and dairy proteins, which can impair gut barrier function. Children with ASD have been reported to experience leaky gut..
Conclusion
Identifying and eliminating foods that trigger sensitivities can alleviate mental health symptoms and enhance overall well-being. While removing certain foods may lead to symptom relief, it’s equally important to maintain a balanced and nutritious diet to support overall physical and mental health.